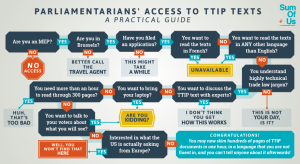
As negotiations continue between Europe and the US on the Transatlantic Trade and InvestmentPartnership (TTIP), concerns are mounting among civil society groups over the implications for public healthcare.
The TTIP is an ambitious free trade agreement which seeks to squeeze a profit out of every aspect of the way we live by ‘harmonising’ regulations, removing ‘non-tariff barriers’ to trade and throwing public utilities and services open to unprecedented and unrestricted competition from transnational corporations (1). The European Commission’s High Level Working Group (HLWG) openly states “The goal of negotiations should be to enhance business opportunities through substantially improved access to government procurement opportunities”. The HLWG classifies “subsidies and other privileges granted to state-owned enterprises” as “anticompetitive policy and behaviour” (2). In addition, the strengthened patent and intellectual property protection the TTIP offers pharmaceutical companies could limit developing countries’ ability to take a flexible approach to IP, restricting access to cheaper generic medicines with disastrous consequences for the world’s poor (3).
Most worryingly, the HLWG recommends that “in the services area, the goal should be to bind to the highest level of liberalisation that each side has achieved in trade agreements to date” (4). Simply put, this means all NHS privatisations, including the conveniently timed 2012 Health and Social Care Act, will be permanently enshrined in law. Linda Kaucher of StopTTIP states, “The Health and Social Care Act and its accompanying regulations have been prepared with input from trade bureaucrats with this free trade agreement (TTIP) in mind. When signed, it will make the NHS changes irreversible in practice.” (5)

Over the last three decades, UK governments of both stripes have steadily corporatized NHS management, outsourced ancillary and technical services, converted hospitals into trusts and cut services such as eye care and dentistry. Hospital planning is now conducted not on the basis of patient need, but the need to meet financial targets. In addition, hospitals must earn their keep via ‘payment by results’ (6, 7). After many small steps, the HSC act represents one giant leap for the government. It legalises competitive tendering for all NHS contracts, forces remaining hospitals into trust status and gives a semi-independent quango power to allocate budget; over 80% to go to free-market care providers. The public has long been fed the line that privatisation is necessary to save a ‘failing’ NHS. This has sadly now become a self-fulfilling prophecy: relentless cuts ensure it can no longer meet demand and recourse to private care is, therefore, only expected to increase (8).
These moves have taken place despite the fact that, in the words of Oliver Letwin, privatisation has the potential to produce services of “inadequate and sometimes unsafe quality” (9). Outsourcing of hospital cleaning was blamed for the MRSA epidemic that claimed the lives of 3,440 people in England between 1993 and 2009 (10). Unison raised concerns about the HSC act in 2012 after inadequate follow up at private Clinicenta facilities left some patients with permanent sight damage. “The government’s drive towards NHS privatisation is leaving patients vulnerable to poor care and support at surgery centres like the one at the Lister hospital. It is potentially the tip of the iceberg in terms of the clinical risk of fragmented health services.” (11). Clinicenta has since been paid 53 million to terminate its contract after a series of blunders, including patient deaths (12).
In an attempt to prevent the NHS as we know it disappearing altogether, civil society and activist groups are now calling on MPs and MEPs to request an exemption from the TTIP. However, neither these nor their US counterparts have any influence over negotiations. The EU Commission holds talks on member states’ behalf and our elected representatives are not so welcome at the negotiating table. The opposite is true, however, of the numerous corporate lobbyists currently enjoying access to decision makers.

But it’s not only the NHS that is under threat from the TTIP. In Spain, healthcare workers have been fighting cuts and layoffs since the crisis began to bite in 2008. As in England, a weakened national health service is now struggling to meet demand. Waiting lists for non-urgent procedures are now anything up to a year, and it is not unusual for patients to be discharged immediately following surgery if post-operative treatments can be self-administered at home. Union representatives at a Barcelona hospital said the TTIP was news to them, but were unsurprised, “Money moves everything here”. They classified it as “Ridiculous that while the US is moving away from a healthcare system which has always been its Achilles’’ Heel, they [national politicians] want to take us in the opposite direction”.
The Spanish have always been proud of their national health service. The Sistema Nacional de Salud (SNS) was set up in 1986 to fulfil the constitutional mandate of the right of all to protection of health. The SNS is based on the same principles as the NHS: universal access for all, based on need not ability to pay. As in the UK, policy and budget decisions are taken at local level, but Spain’s autonomous regions enjoy a much greater degree of autonomy (13).
Catalonia, one of Spain’s economic powerhouses, has largely been governed by the Convergencia i Unió (CiU) party since the 1980s, with a neoliberal approach to health policy. It was the first to integrate diverse public and private healthcare resources and entities into a single network for public use: the Public Hospitals Network (XHUP in Catalan). Private or mixed public/private centres in the XHUP receive government subsidies to treat patients (14). The ratio of private to public in Catalonia has traditionally always been 80/20, but the opposite in the rest of the country. Naturally, it is the Catalan model that interested parties would like to see adopted nationwide.

In 1991, the so-called ‘April Report’ detailed a series of steps towards privatisation of the SNS. Widely rejected by professionals, politicians and the public, it was nominally shelved, to be implemented quietly and at “comfortable intervals” (15). It is a testament to the success of this approach that many of its proposals – including private management, increased involvement of insurance companies, patient charges, outsourcing, mixed private and public facilities, consortiums, private finance initiatives, workforce ‘flexibilisation’, etc. etc. – have been successfully introduced over the intervening years. Greatest uptake has been in those regions with conservative governments (16).
Successive laws such as the Foundations Act (1994) and the New Forms of Management Act (1997) have helped to spread the Catalan model to the rest of Spain. The 1997 act was criticised by the Federation of Associations for the Defence of Public Health (FADSP) for its use of ambiguous language and “hazy definitions of conditions of ownership and public control…. of publicly financed health centres” (17). Today, large chains of private hospitals compete with public ones for patients. Many people hold (tax deductable) company insurance policies and choose to access the same doctors through their private practices. However, as with any business that must turn a profit, spending on equipment and staffing in private hospitals does not match that in the public service, with a knock-on effect on quality of care. In addition, patients are at the whim of the insurance companies who can fight shy of complicated or non-cost-effective procedures.
As in England, Spain’s ruling conservative Partido Popular (People’s Party, PP) has not been slow to take advantage of the pressure austerity has placed on an overburdened health service to pursue its privatisation agenda. In April 2012, it passed its own version of the HSC, the Urgent Sustainability Measures Act. This legalised severe cuts to the SNS, including refusal of assistance to unregistered foreigners, and increased prescription charges (including for previously exempt senior citizens) (18). They proceeded to put these and other measures into practice amid accusations of lack of transparency and underhanded tactics: patients in Madrid complained they were misled about public waiting lists when offered the option to undergo certain procedures in private centres, and, in summer 2013, the Association for the Defence of the Madrid Public Health System [ADSPM] accused the regional health ministry of cutting some 2300 beds as a means of encouraging referrals to private centres (19).

However, in an echo of the Lewisham Hospital victory, in 2014 these plans suffered a severe setback when a series of strikes and protests by Madrid healthcare workers and patients culminated in them taking the regional government to court over its plans to outsource management and services at six public hospitals. Campaigners – under the umbrella organisations of the Marea Blanca (White Tide) and the Madrid Association of Specialist Physicians (Afem) – won their case, and regional health commissioner Javier Fernández-Lasquetty was forced to resign. “Not at any time did they show us any studies, either from Madrid or abroad, saying you can get the same healthcare for less money with private management…… We have demonstrated that the public model is the cheapest”, said Patricia Alonso of Afem. “We have demonstrated that you can stop a reform that has neither economic nor scientific arguments….. We have demonstrated with legal, professional and healthcare arguments that not anything goes” (20).
It remains to be seen how the Marea Blanca and its counterparts will rise to the challenge posed by the TTIP. One thing is certain, however, Madrid politicians will have a triumphant “Sí, se puede*” ringing in their ears for quite some time.
*This loose translation of Obama’s ‘Yes, we can’ has become the universal slogan of all Spanish anti-austerity protests.